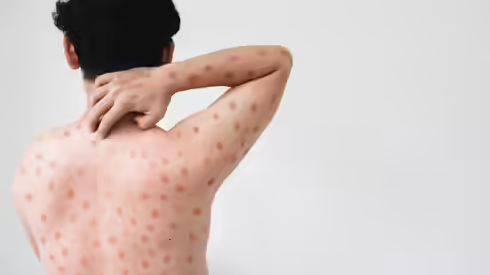
A newly identified strain of mpox, known as clade I mpox-Ib, has been detected in the United Kingdom, drawing renewed attention to the virus due to its historical association with more severe illness. Health authorities stress that the overall risk to the general public remains low, but the strain is being closely monitored because clade I viruses have previously been linked to higher rates of complications and death in some regions.
Mpox, previously called monkeypox, is a viral infection belonging to the Orthopoxvirus genus — the same family as smallpox, though typically far milder. The virus exists in different genetic clades, or families, which vary in severity. The clade II strain, responsible for the global outbreak in 2022, generally caused milder disease and very low death rates. In contrast, clade I, which has been seen mainly in Central Africa, has historically caused more serious illness, particularly among vulnerable populations.
What Is Clade Ib Mpox?
Clade Ib is a sub-lineage within clade I that has now been identified in several countries, including the UK. Current evidence suggests these cases are linked primarily to international travel, rather than widespread community transmission.
Studies reviewing mpox outbreaks between 2022 and 2025 indicate that clade I infections in parts of Africa have shown case fatality rates ranging from 3% to 10%, largely in settings with limited access to healthcare. This contrasts sharply with the well under 1% fatality rate seen during the clade II-driven global outbreak in 2022. Exact death rates specific to the Ib lineage are still being studied, but its classification within clade I has prompted heightened vigilance from health agencies.
Common Symptoms of Clade Ib Mpox
Clinically, clade Ib mpox presents similarly to other mpox infections, according to the World Health Organization (WHO) and UK health authorities. Symptoms usually appear 5 to 21 days after exposure.
Early symptoms often include:
- Fever and chills
- Headache, muscle aches, and back pain
- Swollen lymph nodes, particularly in the neck, armpits, or groin
- Marked fatigue or low energy
Within a few days, a rash typically develops. This rash may:
- Begin as flat spots that turn into raised bumps
- Progress into fluid-filled blisters before crusting over
- Appear on the face, limbs, palms, soles, mouth, genitals, or anus
UK health reports emphasize that many recent cases involve a limited number of lesions, often concentrated in the genital or anal region, rather than a widespread rash. These lesions can be extremely painful. Some patients develop proctitis, an inflammation of the rectum that can cause anal pain, bleeding, and discomfort during bowel movements.
Current Situation in the UK
Since the initial mpox outbreak in 2022, the UK Health Security Agency (UKHSA) has reported sporadic cases, mostly linked to clade II and associated with travel or specific sexual networks. In December 2025, UK authorities confirmed the identification of a clade I–associated mpox case in England, again tied to travel rather than sustained local transmission.
Crucially, no mpox-related deaths have been reported in the UK during this recent period. Globally, WHO estimates that more than 100,000 confirmed mpox cases have occurred since 2022, with several hundred deaths — the majority in regions where clade I circulates and healthcare access may be limited.
Who Is Most at Risk?
Most healthy adults recover from mpox within two to four weeks with rest, hydration, pain relief, and supportive care. However, WHO and recent medical reviews identify certain groups as being at higher risk of severe disease or complications:
- Young children
- Pregnant individuals
- People with weakened immune systems, including those with untreated or advanced HIV
- Individuals with extensive skin involvement or severe anogenital pain
Possible complications include secondary bacterial skin infections, dehydration, pneumonia, eye infections that threaten vision, and in rare cases, sepsis or inflammation of the brain (encephalitis).
How the UK Is Responding
The UK’s response focuses on early detection, isolation, contact tracing, and targeted vaccination. UKHSA treats suspected cases of clade I or Ib mpox as a public health priority, ensuring rapid testing and appropriate follow-up.
Case definitions emphasize symptoms such as compatible rashes or proctitis combined with risk factors, including close physical or sexual contact with a confirmed case or recent travel to areas with ongoing mpox transmission.
The NHS advises anyone experiencing a new, unexplained rash or blisters, particularly around the genitals or anus, along with fever or swollen glands, to seek medical advice promptly.
What This Means for the Public
For most people in the UK, clade Ib mpox remains unlikely, but awareness is important. Recognizing symptoms early — especially painful genital or anal lesions accompanied by fever or swollen lymph nodes — can help prevent further spread and ensure timely care.
Health officials continue to emphasize calm vigilance rather than alarm. Those eligible for vaccination or belonging to higher-risk groups are encouraged to follow NHS and public health guidance closely.